What if many of the conditions we treat as purely psychological or medical problems are actually problems of coordination — of systems that have lost their natural rhythm?
That is the central idea behind a new theoretical framework currently in development in our research group. Drawing on tools from physics, complexity science, and clinical neuroscience, we propose a way of understanding — and potentially reshaping — how the human mind and body organise themselves over time.
Life as an Orchestra
Think of the human body and mind as an orchestra. Your heartbeat, your breathing, your brain activity, your thoughts, your emotions, and even your social interactions all have their own rhythms. In a healthy person, these rhythms don’t all play the same note at the same time — that would be rigid and mechanical. Instead, they coordinate fluidly, coming together and drifting apart as circumstances demand. Like a good improvisation, there is both structure and spontaneity.
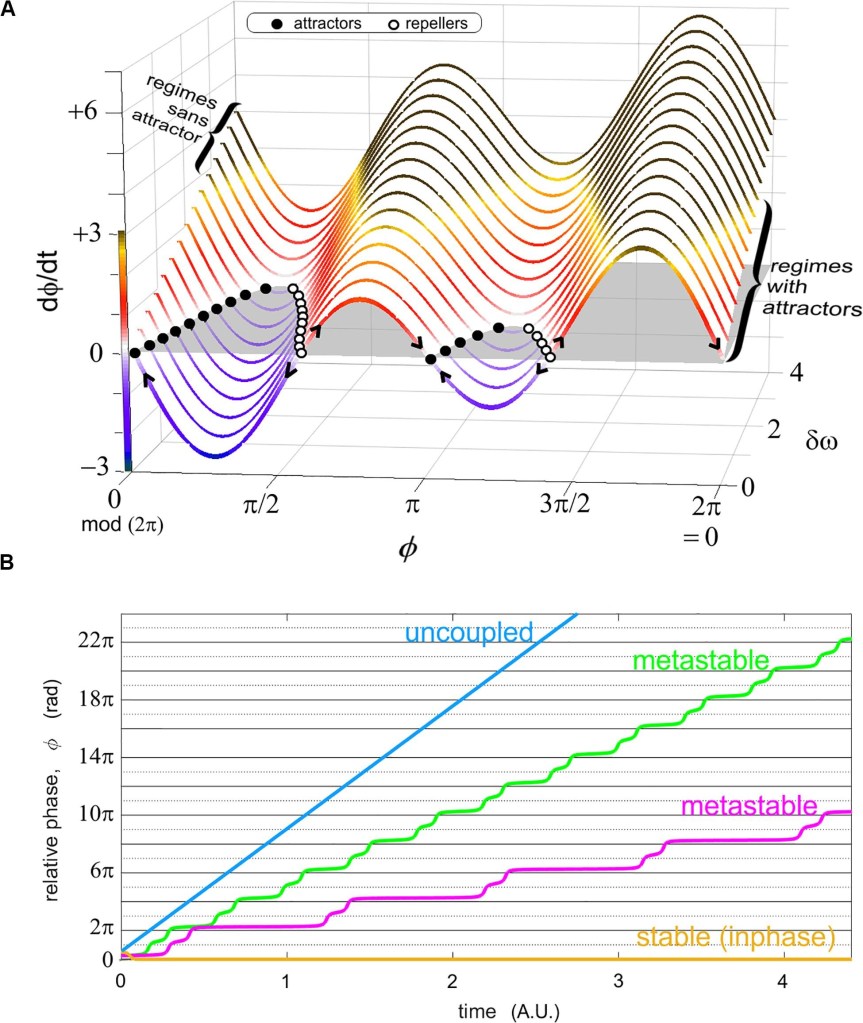
The key concept here is metastability: a state of dynamic balance between order and flexibility. It’s the sweet spot where a system is neither too rigid nor too chaotic — where it can shift smoothly between different patterns without getting stuck or dissolving into noise.
When Coordination Goes Wrong
Many conditions we encounter in clinical practice — from neurological disorders to emotional difficulties to interpersonal struggles — can be understood through this lens as coordination problems. The system doesn’t break in any single component. Rather, the way the components talk to each other becomes dysregulated. Sometimes they become too locked together, too rigid. Sometimes they scatter, losing coherence altogether.
Traditional clinical models often look for what’s wrong with a single part — a neurotransmitter, a thought pattern, a behaviour. Our framework shifts the focus to the relationships between parts, asking: how are neural activity, the autonomic nervous system, cognition, emotion, and interpersonal behaviour coordinating across time?
To capture this, we draw on the concept of chimera states, borrowed from physics. A chimera state is when a system contains both synchronised and desynchronised regions simultaneously — some parts marching in step, others doing their own thing. This turns out to be a surprisingly good description of how healthy human systems actually function. Problems arise when this natural mix gets distorted: too much synchrony, and the system becomes rigid; too little, and it becomes disorganised.
A Mathematical Map for Clinical Practice
We introduce the Coordination Balancing Algorithm (CBA), a mathematical framework that formalises these ideas and translates them into a practical clinical tool.
Rather than aiming to return a patient to a fixed ‘normal’ set point — the traditional homeostatic goal — the CBA aims to restore metastability: the capacity to move fluidly between coordination states as context demands. Health, in this view, is not the absence of change. It is the ability to change appropriately.
The framework uses established tools from nonlinear science — including Recurrence Quantification Analysis and entropy measures — to monitor coordination dynamics in real time. These tools can detect when a system is becoming too rigid or too scattered, and identify the precise moments when it is most open to change (what physicists call critical slowing down near a tipping point). Catching these windows of opportunity can make interventions far more effective — timed to when the system is naturally most plastic and ready to reorganise.
What This Means in Practice
Clinically, this shifts the therapist’s or clinician’s role from ‘symptom reducer’ to ‘landscape navigator’ — someone who uses carefully calibrated interventions to gently reshape coordination patterns in a patient’s system. Instead of pushing a system toward a fixed endpoint, the goal is to expand its repertoire: more accessible states, easier transitions, greater resilience.
This framework applies not just to individuals — it extends to interpersonal dynamics, including coordination between a therapist and patient, between family members, or between any two people engaged in a meaningful interaction.
Looking Forward
This is, at this stage, a theoretical and methodological contribution. The mathematical foundations are robust, and there is encouraging preliminary evidence from multimodal clinical studies. The next step is systematic empirical validation across diverse clinical populations — translating these ideas into tools that practising clinicians can use.
We are working toward that, and we look forward to sharing more as the research develops.
